GENERAL EYE CARE
personalized treatments and services
CLINICAL SERVICES
Our highly skilled clinical doctors, Dr. Michael J. Collins, Dr. Jason C. Friedrichs, Dr. Jay S. Rosen and Dr. Nicole E. Alessi, provide expertise in a wide range of eye care services, from routine exams to the treatment and management of eye diseases. During your visit, our caring, dedicated physicians will explain all of your options and provide you with the information you need to make educated, important decisions about your vision. We look forward to serving you in our Fort Myers and Naples locations.
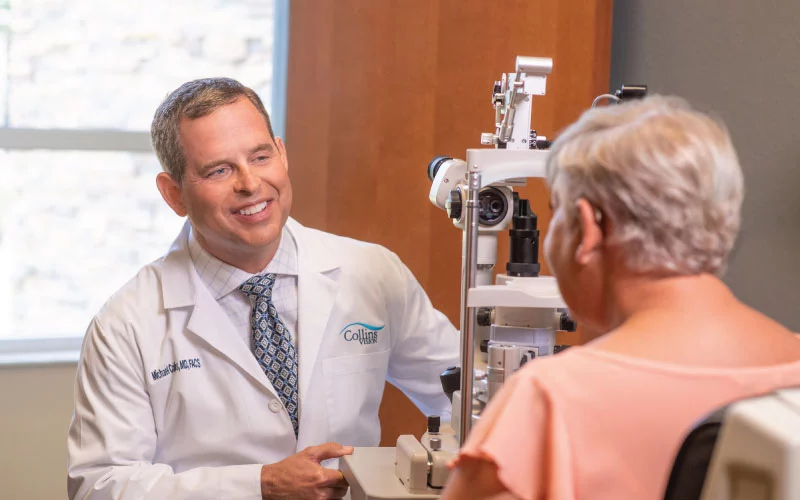
ANNUAL EYE EXAMS
Even if your vision seems “normal”, annual eye exams are an integral part of maintaining the health of your eyes as well as your overall health. Think of your eyes as a window to your entire body; a thorough annual exam can help identify eye diseases like glaucoma, macular degeneration, and cataracts, but it is also able to assist in the early detection of health conditions like diabetes and high blood pressure. The earlier these diseases are detected, the earlier treatment can be started.
CONTACT LENSES & CONTACT LENS FITTINGS
As a part of our commitment to provide various options for superior vision, our optometrists offer the most advanced technology in contact lenses, including specialty contact lenses. In order to maintain the highest level of quality care, the process to obtain a contact lens prescription is the same for both new and existing patients.
COMPREHENSIVE EYE EXAM
The first visit is to examine the health of the eyes; and may be billed as your annual routine eye exam. At this time we will take some basic measurements to get started. We are happy to check with your medical insurance to see if there is coverage for the fitting and contact lenses.
CONTACT LENS FITTING
The goal of contact lens fitting is to find the most appropriate contact lens for each patient’s optimal vision and comfort. With such a wide array of contact lens types, materials, sizes and curvatures, it is critical that a complete fitting and analysis occurs to ensure a proper fit. In some cases, the fitting can be done on the same day as your comprehensive eye exam but, many times, this is scheduled at a later date to allow proper evaluation time.
SPECIALTY CONTACT LENS FITTING
For specialty contact lenses, Dr. Rosen may try several pairs of contact lenses on your eyes from a fitting set. Once he is satisfied with the fit, the next step is to determine the appropriate contact lens power for best vision. Then the lenses are ordered. This visit can take up to an hour or more. On a rare occasion, the doctor may have ordered a pair of contact lenses from the initial measurements, which can be dispensed immediately.
Once the contact lenses come in, the doctor will dispense the contact lenses to you. When the fitting is completed, subsequent visits (if needed) would be billed under your medical insurance. Since this can be a progressive disease, yearly eye examinations are required. If the cornea has changed shape, a new fitting must be repeated.
Keratoconus is a degenerative disease of the cornea. The cornea changes shape (thinning and bulging) often in an irregular fashion, distorting the vision. Sometimes, this irregular shape to the cornea requires “special” contact lenses to enable the patient to see. Although these contact lenses can improve vision significantly, the vision may not be perfect. In fact, a small number of patients require prescription glasses over the contact lenses to improve distance vision. If patients are over forty years old, reading glasses are also needed.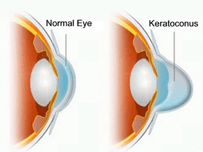
Corneal scarring can occur due to injury or disease. When this occurs the smooth cornea can become bumpy or irregular, distorting the vision. Sometimes, this irregular shape to the cornea requires “special” contact lenses to enable the patient to see. Although these contact lenses can improve vision significantly, the vision may not be perfect. In fact, a small number of patients require prescription glasses over the contact lenses to improve distance vision. If patients are over forty years old, reading glasses are also needed.